Growing older often brings unexpected grooming challenges. This is particularly apparent when some areas that, when young, we could otherwise ignore start to develop hair.
This includes our nose and ears, where hair grows thicker and longer as we age. But why do hairs in these areas act like this?
The answer predominantly lies in our sex hormones.
Two types of hair
There are two types of hair that grows across our bodies.
Vellus hair is fine and colourless. This hair (also called “peach fuzz”) grows across most of our body, including our arms and neck.
Terminal hair is stiff, thick and darker. It stands up from our skin and is usually very obvious. Adult males have terminal hair on about 90% of their body, with females growing it on about 30% of their bodies.
Terminal hair stands up when we’re cold (giving goosebumps) and helps trap heat to keep us warm. It also protects us from the sun (such as hair on our scalp), and keeps dust and dirt out of our eyes through eyebrows and eyelashes.
As vellus hair is smaller, thinner and colourless, it is not usually an aesthetic problem (although it can be altered in some diseases). Instead, it is the terminal hair that is often noticed, and the primary target of our razor.
The normal process of hair development involves a growth phase (anagen), follicle-shrinking phase (catagen), and then a short resting phase (telogen) before the hair falls out and is replaced as the cycle begins again. Some 90% of the hair on our body is in the growth phase at any given time.
Nose, ear, eyelash and eyebrow hairs don’t usually grow too long. This is because the growth phase of the follicles only lasts about 100–150 days, meaning there is a limit to how long they can get.
Alternatively, the hair on your head has a growth phase that lasts several years, so it can grow to more than one meter in length if you don’t get it cut.
Why do we have hair in our nose and ears?
We have about 120 hairs growing in each of our nasal cavities, with an average length of about 1 centimetre.
As you breathe through your nostrils, the hair in your nose works with the mucus to block and collect dust, pollen and other particles that could make their way to your lungs.
The hair in the ears also plays a protective role, trapping foreign objects and working with the earwax to facilitate self-cleaning processes.
What is the effect of ageing?
Androgens are a group of sex hormones that play a key role in puberty, development, and sexual health. The most common androgen is testosterone.
These androgens influence hair growth, and are the key to understanding why we have longer and thicker hairs in our nose and ears.
Hairs in different parts of the body respond to androgens differently. Unlike some hairs that are stimulated at puberty (such as pubic hairs and facial hair in males), some hairs, such as the eyelashes, don’t respond at all to androgens. Others increase hair size much slower, like the ear canal hair that can take up to 30 years.
Females have lower levels of androgens in the body, so major hair growth changes are more localised to the underarms and pubic regions.
We don’t have much data to support various conclusions about hair growth in later life, as most studies have focused on why we lose hair (such as balding) rather than why we have too much.
Nonetheless, there are still some hypotheses about why we grow more ear and nose hair as we age.
As we age, the body is exposed to androgens for a long time. This prolonged exposure makes some parts of the body more sensitive to testosterone, potentially stimulating the growth of hairs.
Over time, and long-term exposure to testosterone, some of the fine vellus hairs may undergo a conversion and become the darker, longer terminal hairs. This terminal hair then sticks out of our noses and ears.
Alongside increased levels of androgens as we go through puberty, a protein called SHBG (sex hormone binding globulin) is also released. This protein helps control the amount of testosterone and estrogen reaching your tissues. During ageing, the levels of SHBG levels may decrease faster than androgens, leaving testosterone to stimulate ear and nose hair growth.
Hair simply changes with age. This can result in changes in colour, thinning, and follicle alterations. There might be variations occurring in the follicles that respond to our body’s changing environment, stimulating longer hair growth.
Most of the impact of hairy ears and noses is observed in males, as they have larger amounts of testosterone.
Should we be worried?
It’s not usually a problem. Having a hairy ear (auricular hypertrichosis) does not appear to impact hearing at all. Note that if you are using hearing aids, excessive hair can impact their effectiveness, so in these rarer cases it is worth having a chat with your doctor.
The largest issue appears to be the appearance of these hairs, which can make some people self-conscious.
To address this, avoid plucking hairs out (such as with tweezers), as this can lead to infections, ingrown hairs and inflammation.
Instead, it is safest to reach for the trimmers (or employ laser hair removal processes) to clean up the area a little.
Christian Moro, Associate Professor of Science & Medicine, Bond University and Charlotte Phelps, Senior Teaching Fellow in Medicine, Bond University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
 Carole Grieg testing the CrossSense AI glasses – SWNS
Carole Grieg testing the CrossSense AI glasses – SWNS Warning appears on the lenses of the CrossSense AI glasses (GNN screenshot of SWNS/CrossSense video)
Warning appears on the lenses of the CrossSense AI glasses (GNN screenshot of SWNS/CrossSense video) Screenshot of Wispy AI in the midst of interacting with user of theCrossSense AI glasses, discussing care of a houseplant (Still from SWNS video)
Screenshot of Wispy AI in the midst of interacting with user of theCrossSense AI glasses, discussing care of a houseplant (Still from SWNS video)





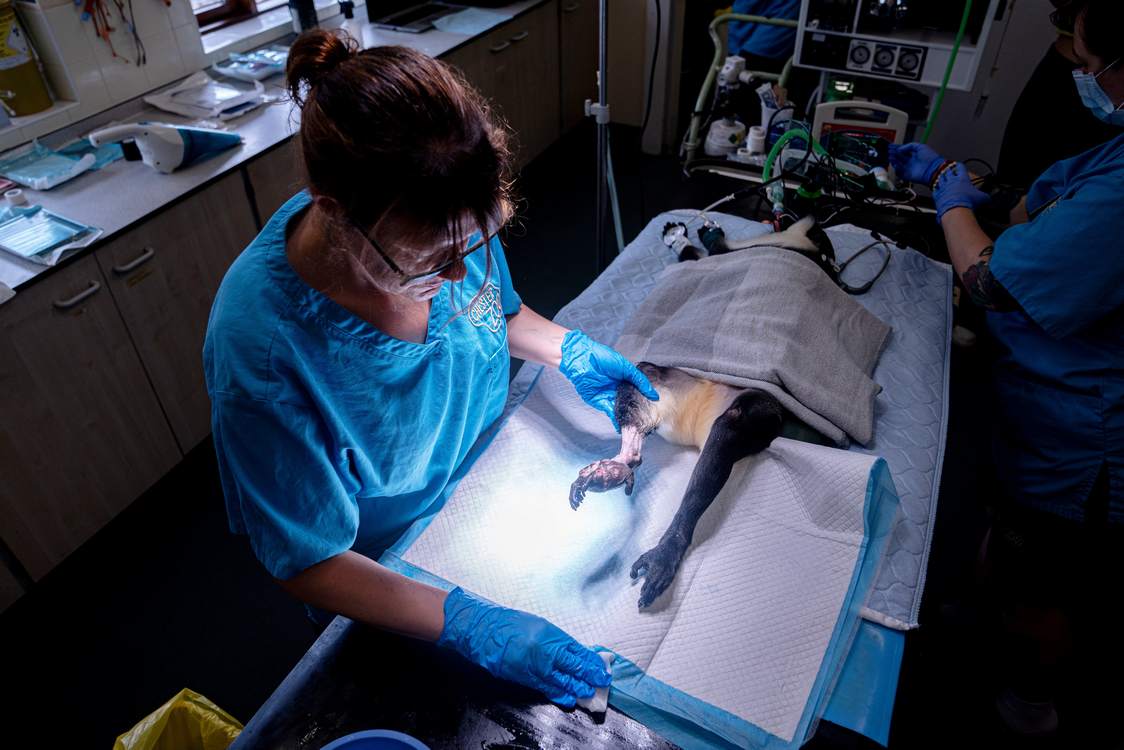 Masaya at the Liverpool Vet. Hospital where she underwent surgery – credit, Chester Zoo via SWNS
Masaya at the Liverpool Vet. Hospital where she underwent surgery – credit, Chester Zoo via SWNS